An artificial pancreas could soon help those people living with type 2 diabetes who also require kidney dialysis. Tests led by the University of Cambridge and Inselspital, University Hospital of Bern, Switzerland, show that the device can help patients safely and effectively manage their blood sugar levels and reduce the risk of low blood sugar levels.
An artificial pancreas could soon help those people living with type 2 diabetes who also require kidney dialysis. Tests led by the University of Cambridge and Inselspital, University Hospital of Bern, Switzerland, show that the device can help patients safely and effectively manage their blood sugar levels and reduce the risk of low blood sugar levels.
Patients living with type 2 diabetes and kidney failure are a particularly vulnerable group and managing their condition can be a challenge. There’s a real unmet need for new approaches to help them manage their condition safely and effectively
Charlotte Boughton
Diabetes is the most common cause of kidney failure, accounting for just under a third (30%) of cases. As the number of people living with type 2 diabetes increases, so too does the number of people requiring dialysis or a kidney transplant. Kidney failure increases the risk of hypoglycaemia and hyperglycaemia – abnormally low or high levels of blood sugar respectively – which in turn can cause complications from dizziness to falls and even to coma.
Managing diabetes in patients with kidney failure is challenging for both patients and healthcare professionals. Many aspects of their care are poorly understood, including targets for blood sugar levels and treatments. Most oral diabetes medications are not recommended for these patients, so insulin injections are the most commonly used diabetes therapy – though optimal insulin dosing regimens are difficult to establish.
A team at the University of Cambridge and Cambridge University Hospitals NHS Foundation Trust has previously developed an artificial pancreas with the aim of replacing insulin injections for patients living with type 1 diabetes. In research published today in Nature Medicine, the team – working with researchers at Bern University Hospital and University of Bern, Switzerland – has shown that the device can be used to support patients living with both type 2 diabetes and kidney failure.
Unlike the artificial pancreas being used for type 1 diabetes, this version is a fully closed loop system – whereas patients with type 1 diabetes need to tell their artificial pancreas that they are about to eat to allow adjustment of insulin, for example, with this new version they can leave the device to function entirely automatically.
Dr Charlotte Boughton from the Wellcome-MRC Institute of Metabolic Science at the University of Cambridge, who led the study, said: “Patients living with type 2 diabetes and kidney failure are a particularly vulnerable group and managing their condition – trying to prevent potentially dangerous highs or lows of blood sugar levels – can be a challenge. There’s a real unmet need for new approaches to help them manage their condition safely and effectively.”
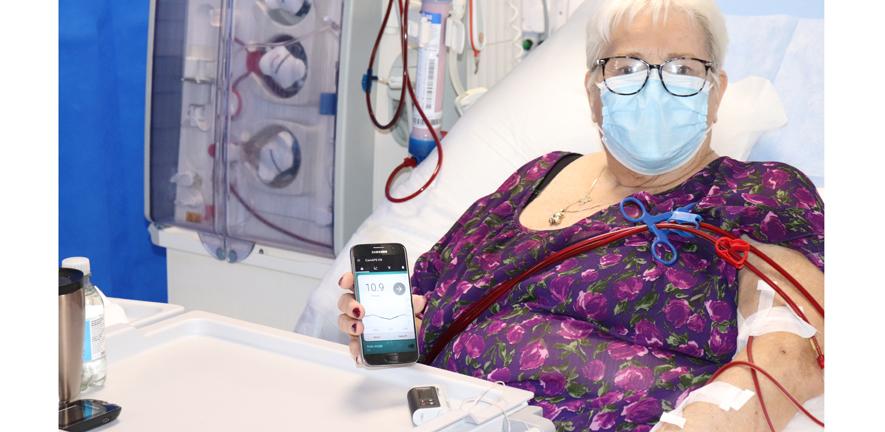
The artificial pancreas is a small, portable medical device designed to carry out the function of a healthy pancreas in controlling blood glucose levels, using digital technology to automate insulin delivery. The system is worn externally on the body, and is made up of three functional components: a glucose sensor, a computer algorithm to calculate the insulin dose, and an insulin pump. Software in the user’s smartphone sends a signal to an insulin pump to adjust the level of insulin the patient receives. The glucose sensor measures the patient’s blood sugar levels and sends these back to the smartphone to enable it to make further adjustments.
The team recruited 26 patients requiring dialysis between October 2019 and November 2020. Thirteen participants were randomised to receive the artificial pancreas first and 13 to receive standard insulin therapy first. The researchers compared how long patients spent in the target blood sugar range (5.6 to 10.0mmol/L) over a 20-day period as outpatients.
Patients using the artificial pancreas spent on average 53% of their time in the target range, compared to 38% when they used the control treatment. This equated to around 3.5 additional hours every day spent in the target range compared with the control therapy.
Mean blood sugar levels were lower with the artificial pancreas (10.1 vs. 11.6 mmol/L). The artificial pancreas reduced the amount of time patients spent with potentially dangerously low blood sugar levels, or ‘hypos’.
The efficacy of the artificial pancreas improved considerably over the study period as the algorithm adapted, and the time spent in the target blood sugar range increased from 36% on day one to over 60% by the twentieth day. This finding highlights the importance of using an adaptive algorithm, which can adjust in response to an individual’s changing insulin requirements over time.
When asked about their experiences of using the artificial pancreas, everyone who responded said they would recommend it to others. Nine out of ten (92%) reported that they spent less time managing their diabetes with the artificial pancreas than during the control period, and similar numbers (87%) were less worried about their blood sugar levels when using it.
Other benefits of the artificial pancreas reported by study participants included less need for finger-prick blood sugar checks, less time required to manage their diabetes resulting in more personal time and freedom, and improved peace of mind and reassurance. Downsides included discomfort wearing the insulin pump and carrying the smartphone.
Senior author Professor Roman Hovorka, also from the Wellcome-MRC Institute of Metabolic Science, said: “Not only did the artificial pancreas increase the amount of time patients spent within the target range for the blood sugar levels, it also gave the users peace of mind. They were able to spend less time having to focus on managing their condition and worrying about their blood sugar levels, and more time getting on with their lives.”
Dr Boughton added: “Now that we’ve shown the artificial pancreas works in one of the more difficult-to-treat groups of patients, we believe it could prove useful in the wider population of people living with type 2 diabetes.”
The team is currently trialling the artificial pancreas for outpatient use in people living with type 2 diabetes who do not need dialysis and exploring the system in complex medical situations such as perioperative care.
Dr Lia Bally, who co-led the study in Bern, said: “The artificial pancreas has the potential to become a key feature of integrated personalised care for people with complex medical needs.”
The research was supported by the NIHR Cambridge Biomedical Research Centre, The Novo Nordisk UK Research Foundation, Swiss Society for Endocrinology and Diabetes, and Swiss Diabetes Foundation and Swiss Kidney Foundation.
Reference
Boughton, CK et al. Fully automated closed-loop glucose control compared with standard insulin therapy in adults with type 2 diabetes requiring dialysis: an open-label, randomised crossover trial. Nat Med; 4 Aug 2021; DOI: 10.1038/s41591-021-01453-z

The text in this work is licensed under a Creative Commons Attribution 4.0 International License. Images, including our videos, are Copyright ©University of Cambridge and licensors/contributors as identified. All rights reserved. We make our image and video content available in a number of ways – as here, on our main website under its Terms and conditions, and on a range of channels including social media that permit your use and sharing of our content under their respective Terms.




