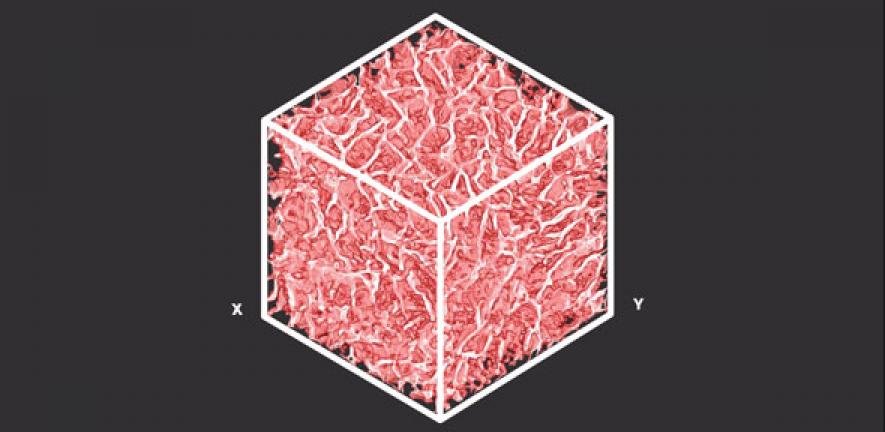
Miniature scaffolds made from collagen – the ‘glue’ that holds our bodies together – are being used to heal damaged joints, and could be used to develop new cancer therapies or help repair the heart after a heart attack.
Miniature scaffolds made from collagen – the ‘glue’ that holds our bodies together – are being used to heal damaged joints, and could be used to develop new cancer therapies or help repair the heart after a heart attack.
We are able to add different types of cells to the scaffold at different times, which no-one else can do
Christine Watson
It may not look like much to the naked eye, but collagen is remarkably strong. The most abundant protein in the animal kingdom, it gives strength and structure to skin, tendons, ligaments, smooth muscle tissue and many other parts of the body.
Through precise manipulation at a structural level, collagen can also be used as a construction material in the laboratory or clinic to help regenerate new tissue, repair damaged cartilage and bone, or aid in the development of new therapies for cardiac disease, blood disorders and cancer.
To understand these conditions better and develop new treatments, or regenerate new tissue, researchers require models that very closely mimic the complex, three-dimensional environments found in human tissue.
As a natural material, collagen is ideal for these biomimetic applications. By shaping it into porous structures, collagen acts as a ‘scaffold’ on which cells and tissue can grow in three dimensions in predetermined forms, mimicking those found in the body.
The idea of using collagen as a scaffold is not new, but the very high level of control that Cambridge researchers are able to achieve over its properties has made a huge range of clinical applications possible, including the repair of damaged joints or tissue, or accelerating the development of new therapies for cancer.
“There is an increasing need for improved materials that work with the systems in the body to regenerate healthy tissue, rather than just replacing what’s there with something synthetic,” said Professor Ruth Cameron of the Department of Materials Science and Metallurgy, who, along with Professor Serena Best, is working with researchers from across the University to develop the scaffolds for a range of clinical applications. “You’re trying to help the body to heal itself and produce what it needs in order to do that.”
To build the scaffolds, the researchers begin with a solution of collagen and water and freeze it, creating ice crystals. As the collagen cannot incorporate into ice, it gathers around the edges of the crystals. When the pressure around the ice is dropped to very low levels, it converts directly from a solid to vapour, leaving the collagen structure behind. By precisely controlling how the ice crystals grow as the water freezes, the researchers are able to control the shape and properties of the resulting collagen scaffold.
By adding small groups of amino acids known as peptide sequences to the surface of the scaffold at different points, the way in which the collagen interacts with the growing cells changes, altering the potential uses for the scaffold. The peptide sequences signal certain cells to bind to the scaffold or to each other, while signalling other cells to migrate. Collectively, these signals direct the scaffold to form a certain type of tissue or have a certain type of biological response.
“The scaffolds are a three-dimensional blank canvas – they can then be used in any number of different ways,” said Cameron, who is funded by the European Research Council. “They can be used to mimic the way in which natural tissue behaves, or they can be directed to form different sized or sequenced structures.”
The technology has already gone from the laboratory all the way to patients, first as Chondromimetic, a product for the repair of damaged knee joints and bone defects associated with conditions such as osteoarthritis, trauma or surgery. By adding calcium and phosphate to the scaffold to mimic the structure of bone, it helps regenerate bone and cartilage. Chondromimetic has been through clinical trials and has received its CE mark, enabling its sale in Europe.
In future, the scaffolds could also see use as a treatment for cardiac disease. Working with Professor Richard Farndale from the Department of Biochemistry and Dr Sanjay Sinha from the Department of Medicine, and supported by funding from the British Heart Foundation, Best and Cameron are developing the scaffolds for use as patches to repair the heart after a heart attack.
Heart attacks occur when there is an interruption of blood to the heart, killing heart muscle. The remaining heart muscle then has to work harder to pump blood around the body, which can lead to a thickening of the heart wall and potential future heart failure.
By modifying the collagen scaffolds with the addition of peptide sequences, they could be used to grow new heart cells to ‘patch’ over areas of dead muscle, regenerating the heart and helping it function normally. Cells could be taken directly from the patient and reprogrammed to form heart cells through stem cell techniques.
While the work is still in its early stages, the scaffolds could one day be an important tool in treating coronary heart disease, which is the UK’s biggest killer. “These scaffolds give cells a foothold,” said Farndale, who is working with Sinha to characterise the scaffolds so that they encourage heart cells to grow. “Eventually, we hope to be able to use them, along with cells we’ve taken directly from the patient, to enable the heart to heal itself following cardiac failure.”
Another potentially important application for the scaffolds is in breast cancer research. By using them to grow mimics of breast tissue, the scaffolds could help accelerate the development of new therapies. Working with Professor Christine Watson in the Department of Pathology, Best and Cameron are fine-tuning the scaffolds so that they can be used to create three-dimensional models of breast tissue. If successful, this artificial breast tissue could assist with the screening of new drugs for breast cancer, reduce the number of animals used in cancer research and ultimately lead to personalised therapies.
“This is a unique culture system,” said Watson. “We are able to add different types of cells to the scaffold at different times, which no-one else can do. Better models will make our work as cancer researchers much easier, which will ultimately benefit patients.”
Like breast tissue, blood platelets also require a very specific environment to grow. Dr Cedric Ghevaert of the Department of Haematology is working with Best and Cameron to use the scaffold technology to create a bone-like niche to grow bone marrow cells, or megakaryocytes, for the production of blood platelets from adult stem cells. In theory, this could be used to produce platelets as and when they are needed, without having to rely on blood donations.
“The technology for culturing the cells is actually quite generic, so the range of applications it could be used for in future is quite broad,” said Best. “In terms of clinical applications, it could be used in almost any situation where you’re trying to regenerate tissue.”
“In some senses, it can be used for anything,” added Cameron. “As you start to create highly organised structures made up of many different types of cells – such as the liver or pancreas – there is an ever-increasing complexity. But the potential of this technology is huge. It could make a huge difference for researchers and patients alike.”
The text in this work is licensed under a Creative Commons Licence. If you use this content on your site please link back to this page. For image rights, please see the credits associated with each individual image.





