Leah Katzelnick was all set for a career as an anthropologist until she contracted dengue fever. She was in hospital for a week with severe symptoms. It changed her life. She is now working on a new perspective on dengue fever which involves mapping the complex interaction between different strains of the virus, based on similar work done by Cambridge experts on flu.
Leah Katzelnick was all set for a career as an anthropologist until she contracted dengue fever. She was in hospital for a week with severe symptoms. It changed her life. She is now working on a new perspective on dengue fever which involves mapping the complex interaction between different strains of the virus, based on similar work done by Cambridge experts on flu.
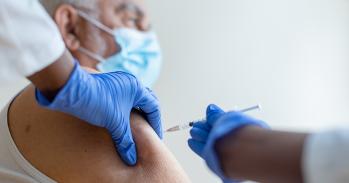
There is no cure for dengue and only the symptoms can be treated
Leah Katzelnick
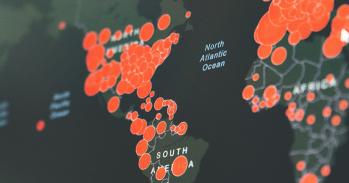
Dengue outbreaks, caused by bites from infected mosquitoes, are common in many developing countries. Four billion people live in areas with the disease, although mortality is relatively low. There are 400 million infections a year: 500,000 people develop severe infection symptoms and approximately 25,000 of these die. However, it places a huge burden on the health services of countries where there are major outbreaks. “Epidemics can swamp public health and intensive care services,” says Leah. “They create fear even if there is a low likelihood of death and in many countries virtually everyone knows someone who has died from it, most of whom are children.”
For her PhD she has been working with both human and non-human primate sera in partnership with the US-based National Institutes of Health. Isolates from some of the main strains of the dengue virus are injected and Leah studies the immune sera to chart the inter-relationship between the four main strains of the virus. Dengue only causes mild infection in the non-human primates she works with.
Leah, who majored in anthropology as an undergraduate in the US, travelled to Nicaragua in her third year as part of a summer fellowship programme on international health. Her aim was to learn about different health systems and beliefs about health. Her research involved talking to people in non-governmental organisations (NGOs) about their aims and talking to people on the ground about how the NGOs were perceived. Then she contracted dengue fever and became very sick and was admitted to hospital.
“There is no cure for dengue and only the symptoms can be treated. In the most mild cases dengue is asymptomatic. Normally people suffer from joint ache, headaches, pain behind the eyes and a strange rash on the hands. In the most extreme cases they suffer from haemorrhagic fever and a rapid drop in platelet count and blood pressure which can cause the body to go into shock. Children who go into shock have a high mortality rate, but if they get good healthcare they can survive,” says Leah.
She spent a week in hospital being monitored for possible shock. Her vascular system was so traumatised afterwards that she felt very weak. The experience led to her doing a lot of research on dengue fever and caused her to rethink her future since people who have been exposed to dengue fever before are more likely to suffer the more extreme form the next time round. As an anthropologist she would have needed to travel and mainly to places where there was dengue fever, but she did not want to risk getting it again.
Leah applied for a fellowship from Williams College in the US to study at Cambridge and spent the summer before in a dengue laboratory in North Carolina estimating transmission of dengue fever in Sri Lanka.
Once at Cambridge, she googled dengue fever research on the university website and the only person she came across who mentioned it was Professor Derek Smith, who studies infectious disease in the Department of Zoology. She read his paper on antigenic cartography and the evolution of flu viruses and felt it could be applied to the four different types of dengue and the complex interaction between those types. She wanted to design an antigenic map for dengue which would show the relationship between the different viruses and how having one might protect you from having that same strain again while having the others could make your feel worse.
She emailed Professor Smith and put her proposal to him. He said there was no funding for a project on dengue. However, Leah’s fellowship allowed her to switch the focus of her studies after a year. That meant she could get funding for a year. She then applied to do a PhD to continue her work and for a Gates Cambridge Scholarship to support her.
Leah began her PhD in 2012 and hopes to complete it next year. She has been working round the clock on her research and says it was initially terrifying since her background was in anthropology rather than lab-based science. Since then she has been presenting her findings at international meetings such as the World Health Organization and has submitted a paper for review to a top journal. She plans to keep working on dengue fever after her PhD is completed and to better understand the human immune response to dengue virus infection so that scientists can limit its impact.
The text in this work is licensed under a Creative Commons Licence. If you use this content on your site please link back to this page. For image rights, please see the credits associated with each individual image.