New treatments for glaucoma are a key priority in vision research. Advances in stem cell technology in Cambridge are helping to make this dream a reality.
New treatments for glaucoma are a key priority in vision research. Advances in stem cell technology in Cambridge are helping to make this dream a reality.
Glaucoma affects more than 60 million people, over 6 million of whom are blind in both eyes.
Glaucoma is the leading cause of irreversible blindness worldwide. Dubbed the ‘silent thief’ because of the insidious manner by which many patients have already suffered significant visual loss before they are diagnosed, glaucoma affects more than 60 million people, over 6 million of whom are blind in both eyes. Currently, the only treatment that can slow the progression of disease is to reduce the eye pressure medically or surgically. However, for some patients, visual deterioration continues unabated even with this intervention. Once vision is lost, it cannot be restored.
Glaucoma has been highlighted as a priority eye disease by the World Health Organization’s global initiative to eliminate avoidable blindness by the year 2020. This recognises the urgent need to find new treatments that can prevent blindness in the most severely affected patients and to restore some useful vision to those blinded by the disease.
Towards stem cell therapy
The potential use of stem cell therapy in the treatment of glaucoma has aroused great interest, and Cambridge researchers are leading the way in this field. Glaucoma involves the progressive death of retinal ganglion cells (RGCs) – the eye cells that carry visual information from the eye to the brain via the optic nerve – and it’s hoped that stem cells can be used to protect surviving RGCs and to replace those that are too damaged to function. This is the goal of Dr Keith Martin and colleagues at the Centre for Brain Repair, who have pioneered a new technique to study the barriers that reduce the survival, migration and integration of stem cells transplanted into the retina.
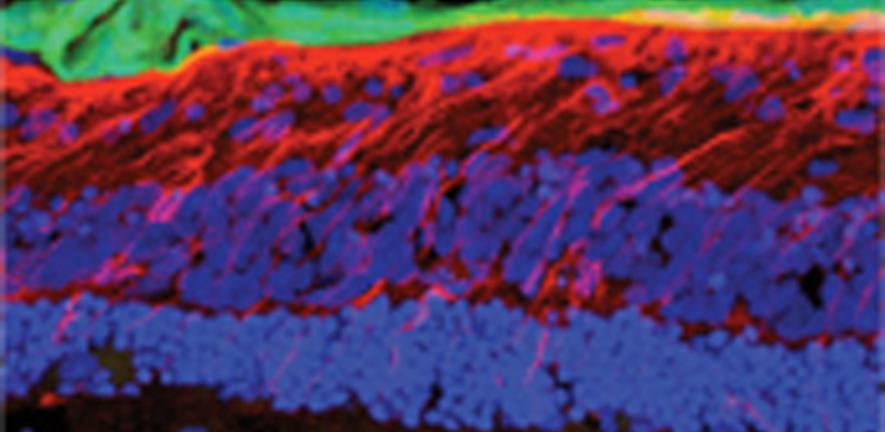
 The model involves the use of a very specific set of tissue culture conditions that enable tissue from a rat’s eye to be kept alive much longer in culture, remaining healthy, maintaining its layered architecture and retaining the ability to make new proteins. The tissue responds to stem cell transplantation in a similar way to that of the eyes of living animals, enabling the researchers to transplant stem cells onto living tissue in a controlled environment and to test treatments to improve integration of the transplanted cells.
The model involves the use of a very specific set of tissue culture conditions that enable tissue from a rat’s eye to be kept alive much longer in culture, remaining healthy, maintaining its layered architecture and retaining the ability to make new proteins. The tissue responds to stem cell transplantation in a similar way to that of the eyes of living animals, enabling the researchers to transplant stem cells onto living tissue in a controlled environment and to test treatments to improve integration of the transplanted cells.
To catch a thief
Replacing damaged RGCs will be a challenging procedure, involving the establishment of complex connections with the retina and brain, and requiring a much better understanding of the inhibitory environment of the mammalian retina. Not only will Dr Martin’s research help to understand the barriers that prevent stem cell transplantation, but it will also help to catch the thief in action – by understanding the pathogenic sequence of eye pressure and neurodegenerative events as they occur.
For more information, please contact the author Dr Keith Martin (krgm2@cam.ac.uk) at the Centre for Brain Repair in the Department of Clinical Neurosciences. This research was published recently in Investigative Ophthalmology and Visual Science and was funded by a GSK Clinical Fellowship to Dr Martin.
Prestigious prize for replacing animal use
Dr Keith Martin and PhD student Thomas Johnson were recently awarded a major prize by the National Centre for the Replacement, Refinement and Reduction of Animals in Research (NC3Rs) for the UK research that has done most over the preceding two years to replace, refine and reduce animal experiments. Until recently, injecting cells into the eyes of anaesthetised animals has been the only way to understand the barriers that prevent the integration of transplanted stem cells into the retina. The £10,000 GlaxoSmithKline (GSK)-sponsored prize recognises the fact that this new retinal culture system allows much of this work to be carried out without the need for animal procedures.
This work is licensed under a Creative Commons Licence. If you use this content on your site please link back to this page.