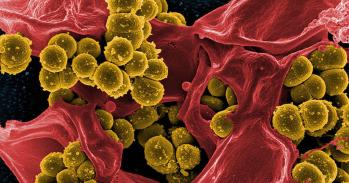
Scientists who recently discovered a new strain of superbug have now tracked its transmission between animals and humans.
Scientists who recently discovered a new strain of superbug have now tracked its transmission between animals and humans.
We can’t predict how these bacterial strains will evolve – they could become more resistant, more virulent or better able to jump between species
Mark Holmes
Every so often, research laboratories and hospitals testing patients for the superbug methicillin-resistant Staphylococcus aureus (MRSA) have come across an oddity: a strain that appeared to be MRSA because it was resistant to antibiotics but one that tested negative with the ‘gold standard’ molecular test. The quirky cases were so infrequent that they were usually filed away for future analysis or disregarded. Until, that is, PhD student Laura Garcia-Alvarez from Cambridge’s Department of Veterinary Medicine had the tenacity to look a little further at a bacterial strain she had spotted in cows’ milk.
MRSA first appeared in 1961 and epidemic strains of this difficult-to-treat bacterium have since spread worldwide in hospitals and the community. In the farming world, MRSA causes bovine mastitis – an infection of cows’ udders – affecting both animal welfare and milk yields.
Garcia-Alvarez was working with Dr Mark Holmes on bovine mastitis when she came across one of the ‘curious anomalies’. The strain was resistant to antibiotics but in the standard molecular test was negative for the presence of mecA – the gene responsible for methicillin resistance. She had the isolates retested and then sequenced at the Wellcome Trust Sanger Institute.
It turned out that she had discovered a new strain of MRSA. Its antibiotic resistance is carried not by mecA but by mecC, a gene that is so genetically dissimilar to mecA that it can’t be picked up by the standard molecular test used to define MRSA but only by DNA sequencing.
As Holmes and Garcia-Alvarez began to spread the information to colleagues around Europe, it soon became clear that this phenomenon was not confined to cows: others had found the unusual samples in humans. “We started to get calls from hospitals and research groups who had come across a small number of human MRSA strains that behaved differently,” said Holmes. “Within a few weeks, we had a further 50 isolates. This meant that what we were looking at was a human problem too.”
Garcia-Alvarez, who at the time was a student on the Department’s postgraduate training in infectious disease dynamics programme, described how finding the same new strain in both humans and cows was worrying, although no cause for immediate alarm: “Pasteurisation of milk will prevent any risk of infection via the food chain. In the wider UK community, less than 3% of individuals carry MRSA – typically in their noses – without becoming ill.”
“Nonetheless,” added Holmes, “MRSA presents a major challenge to the control of infectious diseases. Finding a new strain – studying its prevalence, how it confers antibiotic resistance and how it’s transmitted – can tell us enormous amounts about the origins and evolution of antibiotic resistance.”
New understanding
Since the discovery, Holmes’ team has been investigating the prevalence of the strain in human and animal populations – and the potential for passing the strain between species – in partnership with Cambridge’s Department of Medicine, the Sanger Institute and the Moredun Research Institute (Scotland), and funded by the Medical Research Council.
One of their first steps was to develop a better genetic test, one that also detected the new strain. The timing was fortuitous. Moves to help hospitals identify MRSA more quickly have resulted in the development of automated systems based on genetic testing. Because the standard genetic test does not detect the new strain, the scientists have now developed a protocol that will pick up both strains.
Moreover, their recent research has shown that additional MRSA strains have emerged that possess other mechanisms of antibiotic resistance: “We’ve found about 40 human MRSA isolates that don’t have a mecA or a mecC gene, and we are trying to establish why these are resistant to methicillin-family antibiotics. In retrospect, it was incredibly lucky that the original isolate we investigated happened to have a genetic variation in a known gene that could be picked up by whole genome sequencing.”
To identify how mecC confers antibiotic resistance, Holmes collaborated with Professor Alexander Tomasz at Rockefeller University, New York. They discovered that the gene is more resistant than mecA to cefoxitin (one of the newer classes of antibiotics): “Inappropriate use of antibiotics in human and veterinary medicine has favoured the selection and growth of antibiotic-resistant microorganisms,” explained Holmes. “Our finding suggests that an increased use of this drug may have driven emergence of the new strain.”
“We also now know that the new strain is found in almost every species that we’ve studied, including domestic cats and dogs, wild rats, deer, a rabbit, a common seal, sheep and a chaffinch. The bacterium may have lost factors that restricted it to certain species, or gained pan-host virulence factors that make it better able to colonise multiple species. We need to know how and why this has happened to understand the emergence of bacterial pathogens from animals and their dissemination into human populations.”
Now, their latest research has tracked transmission of the superbug, providing the first direct evidence of transmission of the new strain between livestock and humans.
The researchers capitalised on a growing trend to use increasingly rapid and affordable DNA sequencing for tracking the transmission of pathogens. This technique is helping scientists to look for differences at the level of single letters in the genetic code as a means to map the direction of infection – from patient to patient, and from one animal species to another. The team investigated two cases of mecC MRSA in Danish farmers. The strains circulating in the farmers’ livestock and those isolated from the patients only differed by a small number of letters – strong evidence that the farmers had acquired their infections from their animals, in one case a sheep and in another a cow.
“The ability to confirm animal-to-human transmission in virtual real time using this technology can’t be underestimated,” said Holmes. “High-throughput DNA sequencing is going to revolutionise clinical microbiology by enabling targeted epidemiological follow-up and infection control.”
Nearing the precipice
Mastitis is the most common infectious disease of dairy cattle, affecting the welfare of cows and, according to one estimate, costs the UK dairy industry around £170 million per year. Its control and treatment relies on the use of millions of doses of therapeutic and prophylactic antibiotics every year. “Our research on MRSA is pointing to the fact that although we are not on the precipice of having the whole system collapse through selection of bugs that are even more resistant or having husbandry systems that make it impossible to eliminate them, we are closer to the precipice than we would like to be,” said Holmes. “As it is, S. aureus is considered impossible to eliminate in dairy herds – you have to live with it once you’ve got it. “Farmers and veterinarians are in a constant battle to improve the health of dairy cows, yet farming cannot be sustained at these levels if it is generating these types of resistance. Moreover, we can’t predict how these bacterial strains will evolve – they could become more resistant, more virulent or better able to jump between species.”
Holmes views the interface between veterinary medicine and human medicine as crucial to understanding infectious diseases such as MRSA: “There is very little research on S. aureus mastitis in cows in comparison to research into it as a human pathogen, and yet now we’re beginning to see exactly the same organism being found in people and in cows. This means that we should be thinking about the epidemiology of disease control and the development of antibiotic resistance in both species. Understanding how new strains emerge will help us to understand the growing public health problem of antibiotic resistance.”
For more information, please contact Louise Walsh at the University of Cambridge Office of External Affairs and Communications.
This work is licensed under a Creative Commons Licence. If you use this content on your site please link back to this page.